Ependymoma in children
Ependymomas usually start from ependymal cells. These cells line the fluid filled areas of the brain (ventricles) and the spinal cord.
Ependymomas are most common in children under 5 years old. They are also more common in boys than in girls.
Around 30 children are diagnosed with ependymoma every year in the UK.
Where do ependymomas start in children?

In children, around 70 out of every 100 ependymomas (around 70%) occur in the cerebellum. This is also called the posterior fossa.
About 25 out of every 100 ependymomas (about 25%) develop in the upper part of the brain. This is called the supratentorial area and contains the:
- cerebrum
- choroid plexus
- pineal gland
- hypothalamus
- pituitary gland
- optic nerve
Some children have ependymomas that develop in the spinal cord. But this is much less common.
Ependymomas can also spread into the fluid that surrounds the brain.
Risks and causes
Most people worry about what caused their child to develop cancer. We don’t know what causes most childhood cancers, or how to prevent them. This includes ependymoma.
We know that there’s a small increased risk of ependymoma with some inherited cancer syndromes.
Rarely ependymoma is linked to:
- familial adenomatous polyposis (FAP) - sometimes known as Turcot syndrome
- spinal tumours in neurofibromatosis type 2 (NF2)
But remember, not every child with one of these syndromes develops a brain tumour.
Signs and symptoms
Some children may have symptoms for a few weeks or months before they’re diagnosed with ependymoma. Many symptoms are general and non specific. Some are similar to less serious childhood illnesses. Symptoms will depend on where the tumour is. They can include:
- headaches
- feeling or being sick
- loss of balance
- seizures (fits)
- head tilt
- irritability
- lacking energy
- not gaining weight as they should (failure to thrive)
- neck pain
- speech problems
- coordination problems
- eyesight problems such as double vision, problems moving their eye, or changes to their pupil size
- arm and leg weakness
- not being able to control when they pass urine or poo
Young infants might have an increasing head circumference. A health professional measures this during their well baby check ups. Or the soft spot on top of the skull (fontanelle) might be swollen.
Tests
The first tests your child might have are:
- an MRI scan
- a CT scan
They might also have a lumbar puncture, but this is usually done after surgery. A lumbar puncture is a test to check for cancer cells in the fluid that surrounds the brain and the spine. This fluid is called cerebrospinal fluid (CSF). Your child’s doctor or specialist nurse will take a sample from the fluid around their spine.
For some types of test, including a lumbar puncture, your child might need  or a
or a  . This is to help them lie still.
. This is to help them lie still.
Types and grades
For most types of brain tumours doctors usually look at the cells under a microscope. This usually gives the doctor an idea if the tumour is slow or fast growing. This is called the grade. But for ependymomas, the appearance of cells under the microscope does not always fit with their behaviour. So, the grade may not tell you much about how likely the tumour is to grow or spread.
Researchers are learning more about ependymoma all the time. As a result, ependymoma is now grouped by what the cells look like under a microscope and where the tumour is in the brain. They have also picked up changes (mutations) in the tumours to help understand them more.
There are 4 main types of ependymoma. These are:
- Posterior fossa ependymoma – this is the most common type
- Supratentorial ependymoma
- Spinal cord ependymoma
- Subependymoma – this is a slow growing tumour and is more likely to affect adults than children
Some of these types are further divided into sub types. These depend on changes to  in the tumour.
in the tumour.
Talk with your child’s doctor about their type of ependymoma. And what this means for your child’s treatment plan.
Decisions about treatment
Your child’s specialist team decides on the best treatment options for your child. The team will involve you and your child in the decisions about treatment and care.
The treatments are usually the same for all types of ependymoma.
The most common treatments are:
- surgery
- radiotherapy
- chemotherapy
Some tumours cause a fluid build up in the brain (hydrocephalus). This can cause symptoms. Some of the symptoms might include:
- headaches
- feeling or being sick
- seizures (fits)
- problems with their eyes or vision
- problems with their strength, balance or coordination
- changes in their behaviour
Treatment to reduce this fluid build up is an operation. Your child’s neurosurgeon can do this at the same time as removing the tumour, but they might do it before. They either:
- make a hole to drain fluid into another area of the brain (ventriculostomy)
- put a tube called a shunt in, so that the fluid drains from the brain to another part of the body. This is usually the tummy (abdomen) where the body gets rid of it
Surgery
The exact type of surgery your child needs depends on where the ependymoma is in their brain. The surgeon will aim to remove as much of the tumour as possible during surgery. Your child will have a scan after surgery. Some children might be able to have more surgery to remove more of the remaining tumour.
Hearing that your child needs brain surgery (neurosurgery) can feel very scary. We have more information written for parents and carers about this type of surgery.
Radiotherapy
Radiotherapy treatment uses high energy x-rays to destroy the cancer cells. Your child might have radiotherapy after surgery. This is to reduce the risk of the tumour coming back.
Your child is more likely to have radiotherapy to the whole brain and spinal cord if the fluid around the brain (cerebrospinal fluid) has cancer cells.
If there are no cancer cells in the cerebrospinal fluid, your child might have radiotherapy just to the area of the tumour (and not the spinal cord).
Very young children are more likely to develop side effects from the radiotherapy. So, these children usually have chemotherapy instead of radiotherapy after surgery.
It’s unlikely that your child will have radiotherapy if they are under 3 years and they have a tumour in the area of the brain that contains the cerebrum (supratentorial area). Children over 18 months might have radiotherapy, if they have a tumour in an area called the posterior fossa.
Proton beam therapy
Proton beam therapy is a type of radiotherapy. It uses protons rather than high-energy x-rays to kill cancer cells. Protons are tiny parts of atoms. They work differently from x-rays. They produce a sudden burst of energy when they stop, which stays inside the tumour. The aim is that there is less damage to healthy cells around the tumour.
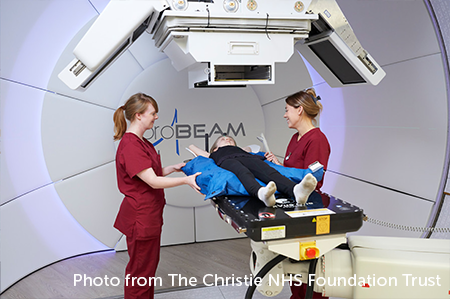
Research shows that proton beam therapy can work well for some types of children’s brain tumours. This includes some, but not all, children with an ependymoma.
Your child’s specialist will talk with you if proton therapy might be helpful for your child.
There are 2 therapy centres in the UK and these are at:
- The Christie Hospital in Manchester
- University College London Hospital
University College London Hospital opened in 2021. They’re gradually opening their service to the rest of the UK. At the moment, children who need this service will have to travel to one of these hospitals or abroad.
Chemotherapy
Chemotherapy is the use of anti cancer drugs to destroy cancer cells.
Some children have chemotherapy after their radiotherapy. This depends on how much of the tumour the neurosurgeon was able to remove. They usually have a combination of a few chemotherapy drugs. This includes some of the following:
- vincristine
- cisplatin
- cyclophosphamide
- etoposide
- carboplatin
- methotrexate
Children under 18 months usually have chemotherapy instead of radiotherapy after surgery. This is because they are at higher risk of severe side effects from radiotherapy during and after treatment. Doctors use chemotherapy to keep a young child's tumour under control, but they may have radiotherapy when they are a bit older.
Your child usually has chemotherapy as  . A cycle lasts 8 weeks. Your child has 8 cycles. Chemotherapy treatment for your child lasts just over a year.
. A cycle lasts 8 weeks. Your child has 8 cycles. Chemotherapy treatment for your child lasts just over a year.
Treatment for ependymoma that has come back
It is more difficult to treat ependymoma that has come back. Treatment depends on what your child had first time round. Depending on the situation they might have:
- surgery to remove the tumour or get rid of as much of it as possible
- radiotherapy
- chemotherapy
Or they may suggest your child has treatment through a clinical trial.
Your child’s specialist will talk with you about the possible treatments for your child. They will involve you in any decisions about their treatment and care. Ask them any questions you have.
Side effects of treatment for ependymoma
The side effects of treatment are different for each child. Some side effects of chemotherapy and radiotherapy happen during treatment and go away once treatment is over. Other side effects happen months or years after treatment. These are known as late effects or long term effects. They can be mild or more challenging. Not all children have challenging long term side effects.
A team of specialists closely monitors your child after treatment. This is to help with any long term side effects.
The side effects of radiotherapy might lead to problems at school or with your child meeting their developmental milestones.
We have detailed information on follow up and late effects of treatment, what treatments can help and where to get support.
Clinical trials
Researchers want to find new and kinder ways to treat ependymoma. And ways to reduce the side effects of treatment. Many children have their treatment for a brain tumour as part of a clinical trial.
SIOP Ependymoma Program II
One trial called SIOP Ependymoma Program II is looking at 3 separate questions to try and improve treatment for ependymoma. They’ve split these into pathways 1, 2 and 3.
Pathway 1 is looking at radiotherapy and chemotherapy after surgery. Half the children and young people taking part will have just radiotherapy. The other half will have chemotherapy after radiotherapy.
Pathway 2 is looking at giving chemotherapy before radiotherapy. Doctors usually treat ependymoma by removing it with surgery. Afterwards they might give radiotherapy to where the tumour was. It’s thought that giving chemotherapy before radiotherapy might help those children whose tumour wasn’t completely removed by surgery.
For pathway 3, doctors want to know if they can improve ependymoma treatment by adding a drug to standard chemotherapy. It’s to help those who can’t have radiotherapy. The drug is valproic acid. We know from research that valproic acid can help people with other types of brain tumours.
The aims of this trial are to find out:
- how well chemotherapy after surgery and radiotherapy works to stop ependymoma coming back
- how well vincristine, etoposide, cyclophosphamide and high dose methotrexate works to treat ependymoma
- how well chemotherapy with valproic acid works for those who can’t have radiotherapy to treat ependymoma
- about the side effects of each of these new ways of treating ependymoma
- how safe these new treatments are
Coping when your child has a brain tumour
We have information about where to get help and support when your child has a brain tumour.



