Surgery to remove lymph nodes from your armpit
You might have surgery to remove most or all the lymph nodes in the armpit (axilla) close to the breast. This is called an axillary lymph node dissection (ALND) or axillary clearance.
Breast cancer can spread to other parts of the body. If it does spread, it usually first spreads to the lymph nodes in the axilla.
What are lymph nodes?
Lymph nodes are small bean shaped structures that are all over the body including near the breast. They are responsible for filtering the lymph fluid as it passes through them. The lymph nodes in the armpit drain the lymphatic fluid from the breast and arm.
It is important to know if there are cancer cells in the lymph nodes in the armpit and how many lymph nodes are affected. This helps the doctors work out the  of your cancer and plan the best treatment for you.
of your cancer and plan the best treatment for you.

Checking the lymph nodes before surgery
Before your surgery you have an ultrasound scan to check the lymph nodes in the armpit close to the breast. This is to see if they contain cancer cells.
You usually have a biopsy of any lymph nodes that look abnormal. The biopsy is sent to the laboratory to check for cancer cells.
If this shows that the cancer has spread to the nodes in the armpit, you will have surgery to remove all or most of them. You have this at the same time as your breast surgery. This is called an axillary lymph node dissection (ALND) or clearance.
You have a sentinel lymph node biopsy instead if either the:
- lymph nodes look normal during the ultrasound scan
- results of an ultrasound guided biopsy shows no cancer cells
Checking lymph nodes during surgery (sentinel lymph node biopsy)
The sentinel node is the first node in the armpit, where the fluid drains into from the breast. This means it’s the first lymph node the breast cancer could spread to. Your surgeon usually carries out a sentinel lymph node biopsy during the operation to remove your breast cancer. You have about 1 to 3 nodes removed to see if they contain cancer cells.
How you have a sentinel lymph node biopsy
You might have your sentinel lymph node biopsy with either:
- a radiotracer and blue dye
- the Magtrace and Sentimag system
Checking with a radiotracer and blue dye
A few hours before the operation, you have an injection of a small amount of mildly radioactive liquid into your breast close to the cancer. You usually have this in the nuclear medicine department in the hospital. The radioactive liquid is called a tracer.
During the operation, your surgeon may also inject a small amount of blue dye into the breast. The dye and the tracer drain away from the breast tissue into nearby lymph nodes.
The surgeon can see which group of lymph nodes the dye reaches first. They also use a radioactive monitor to see which group of lymph nodes the tracer gets to first.
Your surgeon removes between 1 to 3 nodes. They are sent to the laboratory to be looked at by a specialist called a pathologist.
The dye can stain your breast slightly blue. It gradually fades over a few weeks or months. The dye also turns your urine green for a few days.
Checking using the Magtrace and Sentimag system
In some hospitals surgeons use the Magtrace and Sentimag system to find sentinel lymph nodes. It’s usually in the hospitals that have limited access to or are without a nuclear medicine department. Or sometimes as a second (back up) system.
Magtrace is a magnetic liquid tracer that is dark brown in colour. The surgeon injects the tracer into the breast tissue around the cancer. It acts as a magnetic marker and dye. The  in the area soaks up the injected liquid and it gets trapped in the sentinel lymph nodes.
in the area soaks up the injected liquid and it gets trapped in the sentinel lymph nodes.
You can have Magtrace up to 30 days before your operation.
During your operation the surgeon uses a probe called a Sentimag to detect the magnetic liquid trapped in the sentinel lymph nodes. The liquid also acts like a brownish dye so the surgeon can see where it is trapped. The surgeon can then remove the sentinel lymph nodes for testing.
What happens after a sentinel node biopsy?
If the lymph nodes do not contain cancer cells, you won’t need to have any more nodes taken out.
If cancer cells are in the sentinel nodes, you have an axillary lymph node dissection or axillary clearance. This is a second operation that you generally have about 2 weeks after you get the results.
Radiotherapy instead of surgery
Radiotherapy means the use of radiation, usually x-rays, to treat cancer. Some people have radiotherapy to the armpit to destroy any remaining cancer cells instead of surgery.
Getting the results during surgery
In some hospitals, the surgeon gets the results of the sentinel lymph node biopsy during the operation. This is called an intra operative assessment. They can remove the rest of the nodes (axillary lymph node dissection) if necessary. You then avoid having a second operation. This type of testing is called one step nucleic acid amplification (OSNA).
Your surgeon will explain this to you before your operation, so you know what to expect.
Removing most or all of the lymph nodes
You might have this operation as part of your breast surgery or as a separate operation.
You have a general anaesthetic for this operation. You will be asleep the whole time.
The surgeon makes a small cut in your armpit to remove the lymph nodes. Generally, they remove between 10 and 15 lymph nodes. But the number of nodes in the armpit varies from person to person.
The surgeon sends the lymph nodes to the laboratory to check them for cancer cells. You get the results at your follow up appointment.
What happens after surgery?
After the operation, you usually wake up in the recovery room before moving back to your ward or day unit. Find out what else to expect immediately after surgery.
Follow up after surgery
You have follow up appointments to check your recovery and sort out any problems. They are also your opportunity to raise any concerns you have.
You usually see your surgeon one to two weeks after your operation. They examine you and check your wound is healing well.
Your surgeon will explain the results of your surgery and talk about any further treatment you might need.
You'll have contact details of your breast care nurse or the ward if you need to contact someone before your follow up.
Problems after removing lymph nodes
There are some possible problems after having surgery to the lymph nodes in your axilla. Not everyone will have these but there is a bigger risk if you have an axillary dissection. Some of these problems include:
A swollen arm or hand
You are at risk of long term swelling (lymphoedema) in your hand and arm after surgery to remove your lymph nodes in the armpit. This is swelling caused by lymph fluid that can't drain away. It can happen any time after surgery and radiotherapy to your armpit.
Not everyone will get this and it is less likely to happen if you only have a few nodes removed. But it is very important to speak to your specialist nurse or surgeon if you think your arm or hand may be swollen.
Unfortunately, once you have lymphoedema it can’t be cured. But early treatment can help to control it. Your nurse will talk to you about ways of preventing lymphoedema.
Shoulder stiffness
Your shoulder might become stiff and painful after breast surgery to the lymph nodes.
Your nurse or a physiotherapist will show you exercises to do after your operation to help improve movement in the shoulder.
Fluid collecting around the operation site (seroma)
Sometimes fluid collects near the wound and around the armpit. This might happen after your nurse removes the wound drain if you have one.
It can cause:
- swelling
- pain
- an increased risk of infection
The fluid normally goes away on its own within a few weeks.
Your nurse or doctor can drain the fluid with a needle and syringe if the seroma is painful. Sometimes the fluid can build up again after being drained.
Tell your doctor or nurse if you think a seroma is developing.
Wound infection
Tell your doctor or nurse if your wound:
- looks red and swollen
- feels warm
- is painful
- leaks fluid (discharge)
These are signs of infection. You may also feel unwell and have a temperature.
If you have an infection, your doctor will give you antibiotics. You might need to stay in longer or go back into hospital if you need antibiotics through a drip.
Nerve pain
You might have numbness, tingling or a shooting pain in your armpit, upper arm, shoulder or chest wall. This is due to damage to the nerves during surgery. The nerves usually repair themselves, but it can take many weeks or months.
Your doctor or nurse can give you medicines to help with nerve pain.
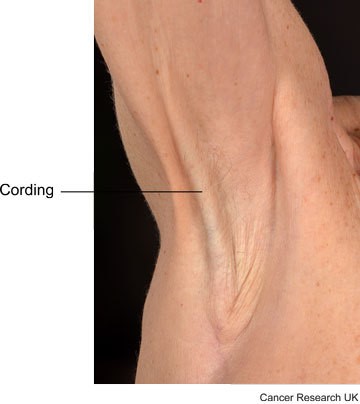
Scar tissue in the armpit (cording)
Some women develop scar tissue in the armpit after lymph node removal. The connective tissues in the armpit get inflamed, which forms one or more tight bands. This usually happens within the first few weeks or months after the operation.
The scar tissue is called cording or banding or axillary web syndrome. It can feel something like a guitar string. It can extend down the arm past the elbow, possibly as far as the wrist or thumb.
Cording is harmless but can be painful and can limit your arm movement. Massaging the area regularly can help. Tell your breast care nurse if you develop cording. They can refer you to a physiotherapist. They can show you how to massage the area and teach you stretching exercises. It usually gets better within a few months. Taking anti inflammatory painkillers may also help. Speak to your nurse or doctor about taking these.