Laparoscopy
Laparoscopy is a small operation to look inside your tummy (abdomen) and the area between your hips (pelvis). Laparoscopy is also known as keyhole surgery or minimally invasive surgery.
It can help diagnose certain types of cancer. It is also a very common procedure used to treat and diagnose many other non cancerous conditions.
A laparoscopy involves your surgeon making several small cuts (incisions) instead of a large incision across your abdomen. The surgeon places hollow tubes inside the incisions. These are called ports.
Your surgeon puts a thin tube with a light and a camera (laparoscope) through one of the ports in your abdomen. Through another port the surgeon passes the tools they will use. There are several tools they might use and this will depend on what your surgeons sees. So for example they may use an ultrasound probe to look at the deeper layers of the tissue inside your abdomen or pelvis. Or they may use a tool to take samples (biopsies) of any abnormal areas in and around your abdomen and pelvis.
You have the operation while you're asleep, so you have a  . A laparoscopy can take from as little as half an hour to a couple of hours.
. A laparoscopy can take from as little as half an hour to a couple of hours.
You usually have a laparoscopy as a day case, so you can go home later the same day.
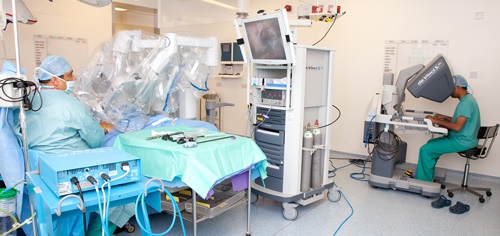
Some laparoscopic operations use a robot. This is called robotic surgery or robotic assisted surgery. This is where the surgeon sits at a console and directs the robotic arms to perform the surgery.
Below is a picture of robotic surgery for prostate cancer.
Why might I have a laparoscopy?
You might have a laparoscopy to diagnose your cancer. This includes cancers that start or spread to the:
- stomach
- pancreas
- liver
- ovaries
- bile duct
- gall bladder
- tummy lining (peritoneum)
Before your laparoscopy
You usually have an appointment before your laparoscopy to check that you’re fit enough for the procedure and to have an anaesthetic. A nurse weighs you and takes your blood pressure, pulse and temperature.
You might also have:
- blood tests to check your blood levels and how well your blood clots
- a heart trace (ECG)
- a chest x-ray
You might meet your surgeon at this appointment or on the day of your operation. They’ll go over the procedure and what to expect, they’ll then ask you to sign a consent form. You can ask any questions you might have.
Preparing for your laparoscopy
Tell your doctor if you’re taking medicine that changes how your blood clots. These include:
- aspirin
- clopidogrel
- arthritis medicines
- warfarin or heparin
- apixaban or rivaroxaban
- ticagrelor
Your doctor tells you if you need to stop your medicines or change the amount (dose) before the laparoscopy. It’s a good idea to take your prescription with them all listed.
You can’t eat for 6 hours before the operation. You might be able to have water for up to 2 hours beforehand. The hospital staff will give you instructions about this.
Tell your doctor if not eating could be a problem for you, for example if you have diabetes.
What happens?
On the day of your laparoscopy you first meet your nurse. They go over your medical history you mentioned at the previous appointment and check if you any allergies. They also take the same measurements such as your:
- blood pressure
- heart rate
- temperature
- oxygen levels (saturation)
Before the operation you’ll meet the surgeon and also the anaesthetist.
You sign a consent form if you haven’t done so already.
You change into a hospital gown when it’s nearer the time to go to the operating room (theatre). It’s a good idea to take along a dressing gown and slippers.
When it’s your turn the nurse takes you to theatre.
In the operating room
You lie on the operating bed and the anaesthetist puts a small plastic tube (cannula) into a vein in the back of your hand or arm. At a similar time other staff in the operating theatre attach some monitoring equipment to you. Such as a blood pressure cuff and clip on your finger to measure your oxygen levels and heart rate.
The anaesthetist then injects the medicine to put you to sleep (anaesthetic) through the cannula. You then drift off to sleep.
The surgeon then makes usually 2 or 3 small cuts. These include:
- one in or near your tummy button
- on one or both sides of your abdomen
Your surgeon first puts gas (carbon dioxide) into your abdomen. This lifts your abdomen off the structures inside your body. It makes it easier for the surgeon to see your organs, including the liver, stomach and gallbladder.
Hollow tubes called ports are placed inside the cuts to hold them open and allow the laparoscope to pass through easily.
Your surgeon puts the laparoscope through one of the cuts. They can see the inside of your abdomen and pelvis on a TV screen. They put other surgical instruments through the other cuts such as an ultrasound probe.
The surgeon looks for signs of cancer in the:
- lining of your abdomen and pelvis
- surface layer of organs in your abdomen and pelvis
Your surgeon might take biopsies and fluid to send to the laboratory to check for cancer cells if they see any abnormal areas.
After they have finished your surgeon removes the instruments and ports. They close the small holes with stitches.
After the laparoscopy
You wake up in the recovery area and then go back to the ward. You might have fluids through a drip into your cannula. Once you’re awake and drinking, your nurse takes the drip out. You should be able to eat and drink normally once you feel able to.
You might have some pain in your:
- abdomen for a few days
- shoulder for a day or two due to the gas in your abdomen
You usually have paper stitches over the wounds (Steri-Strips) or dissolvable stitches. You also have a waterproof dressing over them or a type of special skin glue.
Check with your nurse how long you should keep your dressing on for.
Because you have had an anaesthetic, you’ll need someone to take you home and stay with you overnight. For 24 hours after a general anaesthetic you shouldn’t:
- drive
- drink alcohol
- operate heavy machinery
- sign any legally binding documents
Possible risks
Most people won’t have problems from this type of operation. Your doctor makes sure the benefits of having it outweigh the risks. Some of the possible risks include:
A wound infection
There is a risk of infection at the site where the cuts were made with this operation. Contact your healthcare team if you have:
- a high temperature or feel unwell
- any redness or swelling around your wound or it’s leaking fluid
You will need antibiotics to clear the infection if you have one.
Bleeding
You might notice a small amount of blood from the cuts. This usually heals up on its own. Rarely there might be damage to a major blood vessel. If this happens you might need another operation. You might also need a blood transfusion.
Blood clot
Signs of a blood clot include pain, swelling and redness where the clot is. Feeling breathless can be a sign of a blood clot on the lung.
Contact your advice line or doctor straight away if you have any of these symptoms.
Tummy (abdominal) pain
You may have some cramping or pain in your tummy after the test. This is due to the carbon dioxide they put into the bowel. This should go away after a few hours. You may also experience some pain or tenderness if you had some tissue removed.
Tear in your bowel
Very rarely you might get a small tear (perforation) in the first part of your small bowel. If this happens it’s likely you would need surgery to repair the tear.
Your nurse will tell you what to look out for. They’ll also give you a number to contact if you have any problems.
An allergic reaction
There is a risk of having an allergic reaction to the anaesthetic. This can cause problems with your breathing, heart rate and blood pressure. If this happens, the staff will give you medicines to control the reaction.
Getting your results
One to two weeks after the test you should get the results from your specialist. Waiting for results can make you anxious.
You might have contact details for a specialist nurse and you can contact them for information if you need to. It may help to talk to a close friend or relative about how you feel.
For support and information, you can call the Cancer Research UK information nurses on freephone 0808 800 4040. The lines are open from 9am to 5pm, Monday to Friday.



