Mammogram
A mammogram is an x-ray of your breasts. X-rays use high energy rays to take pictures of the inside of your body.
You might have mammograms:
-
as part of the breast cancer screening programme
-
to check for cancer if you have symptoms that could be due to breast cancer. This is called a diagnostic mammogram
The health professionals who take mammograms are called mammographers. The mammogram itself usually only takes a few minutes, but the appointment may last about 30 minutes.
Mammograms for breast screening
Mammograms for breast screening can help to find breast cancer early when they are too small to see or feel.
Who has breast screening?
The NHS breast screening programme invites all women aged between 50 and 70 for screening every 3 years. You need to be registered with a GP to receive the invitations.
It is important to see your GP if you notice any symptoms between your screening mammograms.
Mammograms to check for breast cancer
You might have a mammogram if you are over 40 and have:
- a new lump or thickening in your breast or armpit
- a change in size, shape or feel of your breast
- skin changes in the breast such as puckering, dimpling, a rash or redness of the skin
- fluid leaking from the nipple if you are not pregnant or breastfeeding
- changes in the position of the nipple
You usually have a mammogram alongside other tests, such as a breast examination and ultrasound scan in a breast clinic. You might also have a sample of tissue (biopsy) taken in this clinic.
Having a breast examination, a scan or mammogram, and a biopsy is known as a triple assessment.
Preparing for a mammogram
There are no special preparations for a mammogram. You can eat and drink normally beforehand.
Avoid using talcum powder or deodorant on the day of your test as this may affect the mammogram.
Tell the mammographer if you have breast implants. You may need extra x-rays taken. The mammographer is very experienced in doing mammograms with women with breast implants.
If you are a transgender or non-binary people who wear a binder, you will need to remove this just before you have your mammogram.
Where will I have my mammogram?
If you are having a mammogram as part of the breast cancer screening programme, you may have it in a mobile unit or in a hospital. Some units are also based in shopping centres.
You usually have mammograms to check for breast cancer in the x-ray department or a specialist breast clinic. This is usually at your local hospital.
What happens
You take off your clothes from the waist upwards. You might put on a hospital gown.
You stand close to the x-ray machine. The radiographer positions one breast at a time between 2 flat plates on the machine. The plates press your breast firmly between them for a few moments. You will feel a little pressure and it is likely to be uncomfortable. Some women find it painful, but it is over quickly.
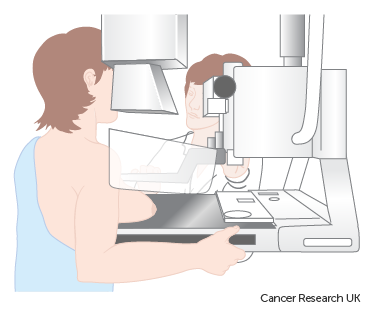
You usually have 2 x-rays from each breast: one from the top and one from the side.
Talk to your mammographer if you are nervous or embarrassed. Or if you are finding the mammogram too painful. They can stop at any time and try to make you more comfortable.
The video below shows what happens during a mammogram. It last around 1 minute.
A mammogram is an x-ray of the breast. It looks for early changes that could be a sign of cancer.
The radiographer positions one breast at a time between two flat plates on the machine.
This compression helps to give a clear picture.
The radiographer takes the x-ray from behind a screen. This protects her from the radiation because she is taking x-rays everyday.
Radiographer Ok, take a step back
They take two pictures of the breast – one from above and one from the side. Then they x-ray your other breast.
Some women find mammograms a bit painful. But most only feel mild discomfort. Either way, it doesn’t last for long.
Your mammogram goes to a specialist radiographer or doctor to look for changes that could indicate breast cancer.
You should get your results within a few weeks.
3D mammograms
This is a detailed type of mammogram that is available in some hospitals. It takes more x-rays than a standard mammogram. A computer uses these to create a 3-dimensional (3D) image of the breast. This is also called digital breast tomosynthesis (DBT).
Contrast enhanced spectral mammography (CESM)
A CESM is a type of mammogram where you have an injection of a dye (contrast medium) into a vein of your arm before taking x-ray images of the breast. This type of mammogram is available in some hospitals.
After your mammogram
You can get dressed straight after the mammogram. You might have some tenderness in your breast for up to a few hours.
Specialists called radiologists look at the mammogram pictures. They check for any abnormal areas.
If everything looks normal you might not need any further tests. Sometimes the mammogram isn’t clear enough, so you may need to have the mammogram again.
If an abnormal area shows on the scan, you have more tests. These may include a breast ultrasound scan or a  . You may have these tests during the same visit in a one stop breast clinic.
. You may have these tests during the same visit in a one stop breast clinic.
Getting your results
You might get the results on the same day. Or you receive a letter with the results within 2 to 3 weeks of having the test.
Waiting for test results can be a very worrying time. You might have contact details for a specialist nurse who you can contact for information if you need to. It can also help to talk to a close friend or relative about how you feel.
Do contact the staff at the clinic if you haven’t heard anything after a couple of weeks.
Possible risks
A mammogram is a very safe test, but with any tests, there are possible risks.
Exposure to radiation
With each mammogram, there is a small amount of radiation exposure from the x-rays. But the amount of radiation is very small.
X-rays can very rarely cause cancer. Having mammograms every 3 years for 20 years very slightly increases the chance of getting cancer over a woman’s lifetime.
Pregnancy
It is very important to tell the mammographer if you think you may be pregnant, as the x-rays could affect your developing baby.
Risks of breast screening
Screening doesn't always find a cancer that is there. So some people with breast cancer will be missed. This is called a false negative result.
For some, a mammogram may pick up something even though they don't have breast cancer. This is called a false positive result and can lead to anxiety and further tests such as a breast biopsy.
It is important to see your GP If you notice any symptoms that could be due to breast cancer.
Angela's breast cancer story
"I'm so pleased I went for my routine mammogram."



