Colonoscopy
A colonoscopy looks at the whole of the inside of the large bowel.
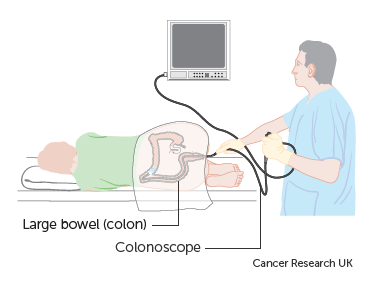
A doctor or nurse (endoscopist) uses a flexible tube called a colonoscope. The tube has a small light and camera at one end. The endoscopist puts the tube into your back passage and passes it along the bowel. They can see pictures of the inside of your bowel on a TV monitor.
Why might you have a colonoscopy
You may need a colonoscopy:
- to help find the cause of bowel symptoms
- to look for early signs of bowel cancer as part of the national bowel cancer screening programme
- to look for early signs of bowel cancer if you are at high risk of developing bowel cancer
- as part of your follow up after treatment for bowel cancer
- to look further into an abnormality found on another test such as a CT scan
Preparing for a colonoscopy
You need to have an empty bowel for the test. This is so the endoscopist can clearly see the inside of your bowel.
To empty your bowel you take medications (laxatives) the day before your test.
After taking the laxatives you might need the toilet often and very suddenly. You may have some cramps. It's best to stay at home for a few hours after taking laxatives so that you are near a toilet.
The hospital might ask you to eat a low fibre diet for 1 or 2 days before the test. It is very important to drink plenty of clear fluids. This includes:
- water
- black tea or coffee
- squash (not with red or purple colouring)
- clear soup
If you take iron tablets or other medicines that can make you constipated, you might need to stop these a week before the test.
Contact the endoscopy unit as soon as possible before your appointment if you take medicines to thin your blood or you are diabetic. You'll be given other instructions to follow.
You’ll receive clear instructions about what you can and can’t eat or drink before this test.
What happens
You usually have a colonoscopy as an outpatient in the endoscopy department at the hospital.
Before the procedure you’ll see your endoscopist. They'll explain the procedure to you and ask you to sign a consent form. This is a good time to ask any questions you may have.
You wear a hospital gown and might also wear paper shorts with an opening at the back.
You're offered painkillers and a medicine to relax you, these make you drowsy (sedation). You have these as injections into a small tube (cannula) in your vein. Some hospitals use gas and air (Entonox). This is a fast acting pain relief that you breathe in through a mouth piece.
You lie on your left side with your knees drawn up towards your chest. The colonoscope goes into your back passage (rectum) and passes into your bowel. The tube bends easily so it can pass around the curves in your bowel.
The endoscopist puts a small amount of gas into your bowel. This opens up the bowel to help them see all the bowel lining.
The endoscopist may press on your stomach or change your position to help the tube pass through your bowel.
During the test they take photographs of your bowel lining. And the endoscopist can remove tissue samples (biopsies). If they see any growths (polyps) they remove them with a wire loop put down the colonoscope. You might also have a dye sprayed onto the lining of the bowel to show up any abnormal areas. This is called chromoscopy.
Colonoscopies can be uncomfortable but shouldn't be painful.
Take a look at this short video about having a colonoscopy.
A colonoscopy is a test to look at the inside of your large bowel. Your bowel needs to be empty for the test, so the day before you don’t eat solid food but should continue to drink plenty of clear fluids.
You also take a laxative. This causes diarrhoea so it’s best not to make any plans that day and to stay at home close to a toilet.
On the day you can drink clear fluids until two hours beforehand.
For the test you lie on your left side and you may have some medicine to make you sleepy and some painkillers. Then the doctor puts a long flexible tube called a colonoscope into your back passage and up into your large bowel.
This is uncomfortable and you may have some crampy pains. Concentrating on slow, deep breathing helps. The pain tends to pass quickly.
On the end of the tube is a light and a camera this sends pictures to a monitor.
They take samples of any abnormal looking areas - this is called a biopsy, and remove any small growths called polyps that you may have. These aren’t cancer but if left can sometimes change into it over a number of years.
Afterwards you need to rest while any medicine you have had wears off. You may have some bloating and stomach cramps for a few days.
Your doctor will be able to tell you if they have seen any changes straight away but it will take a week or so to get the results of any biopsies they have taken.
After your test
You go to a recovery area to rest if you have had sedation. Your nurse monitors you. They offer you a snack and drink when you are ready. You might be in the recovery area for a couple of hours.
You might have bloating and cramping pains after the test. This is due to the gas that goes into your bowel. It normally gets back to normal after a few hours.
As you’re having sedation you’ll need someone with you so they can take you home and stay with you overnight. Also for 24 hours after you shouldn’t drive, drink alcohol, operate heavy machinery or sign any legally binding documents.
Possible risks
Colonoscopy is a very safe procedure. But your nurse will tell you who to contact if you have any problems afterwards. Your doctors make sure the benefits of having a colonoscopy outweigh any possible risks.
Some of the possible risks include:
Tummy (abdominal) pain
You may have some cramping or pain in your tummy after the test. This is due to the carbon dioxide or air they put into the bowel. This should go away after a few hours. You may also experience some pain or tenderness if you had some tissue removed during the colonoscopy.
Bleeding
After having a biopsy or polyp removed, you might have some bleeding. This is usually a small amount and stops on its own within a couple of days.
Tear in your bowel
Very rarely there is a small tear in the bowel wall (perforation). If this happens it’s likely you would need surgery to repair the tear.
Difficulty breathing
There is a risk you might react to the sedation drug. It can cause temporary feeling of difficulty with breathing. But this is rare. It's easily treated by giving you oxygen through a small plastic tube into your nose. Your nurse monitors you closely.
Getting your results
Before you go home, your doctor tells you if they removed any growths (polyps) or tissue samples (biopsies) from your bowel.
The biopsy results can take up to 2 weeks. Your specialist writes to you with the results. If your GP referred you for the test, they should also receive a copy. Contact your doctor if you haven’t heard anything after a couple of weeks.
Waiting for biopsy results can be an anxious time. It might be helpful to talk to someone close to you.
More information
We have more information on tests, treatment and support if you have been diagnosed with cancer.



